
21 Nov Healthy vs Unhealthy Gums in Dogs
When it comes to healthy dog gums we often hear the question, “does my dog need a dental?” A dental can mean so many different things. At Animal Dental Care and Oral Surgery, we want to be very specific with an answer to that question. More importantly, we want you to know exactly what is involved with the answer to that question.
A dental is not just a cleaning, but a thorough exam and treatment plan referred to as a Comprehensive Oral Health Assessment and Treatment (COHAT) with multiple steps. These steps have been covered in previous blog posts.
Your Dog’s Gum Health
It has been estimated that by the age of 2 years, 80% of dogs and 70% of cats have evidence of periodontal disease. Periodontal disease is the most common and prevalent disease diagnosed in our pets. The question becomes, “how do we know if our pet has gingivitis or periodontitis?” An easy place to start is with a quick look in our pet’s mouth. Do we see an accumulation of plaque and calculus or evidence of gingivitis (inflamed/irritated/red gum tissue)?
An oral exam on an awake patient is just a glimpse into the mouth. Even in the calmest and most willing patient, it’s impossible to see everything including what lies beneath the gum line. We are just looking for overt evidence of dental disease. Valuable information is still obtained during these exams and can be useful in providing direction on how to proceed.
When looking in the mouth of an awake patient, I am focusing my attention on the gingiva (gums). Outside of other potential problems that need to be addressed, gingivitis and periodontitis are common and likely present. Even in our young pets, evidence of gingivitis and periodontitis can be present.
Signs of Unhealthy Gums
Bad breath (halitosis) and inflamed gums (gingiva) are two common clinical signs noticed by owners. Gingivitis is often the first sign of periodontal disease observed and is limited to inflammation of the gum tissue. Periodontitis is defined as the inflammation and destruction of the bone and soft tissues around the teeth due to plaque accumulation, which then often leads to negative systemic ramifications. These are the tissues that anchor the teeth in the mouth.
As periodontal disease progresses, more and more destruction to these tissues occurs leading to gingival recession, tooth root exposure, bone loss, and eventual mobility and loss of the tooth. On this continuum of periodontal disease, gingivitis is defined as inflammation of the gingiva, and is the only stage of periodontal disease that is truly reversible. With regards to the loss of soft tissue and bone during periodontal disease, once these tissues are lost it is very difficult to regenerate or repair.
Healthy vs. Unhealthy Gums
Knowing that gingivitis is reversible and periodontitis in not, the goal is then to detect dental disease in our patients when the gums are irritated and inflamed before we have tissue destruction and loss. So the question is, “how do we detect gingivitis?” Healthy gum tissue typically has a coral pink color. Many dogs have dark pigment in these tissues that may be interspersed with the coral pink tissue. In addition, the gingiva should be smooth and surround each tooth, attaching just below the crown. And the margin of the gingiva should surround the crown and create a shallow sulcus or groove. This groove is the battlefield where plaque begins to accumulate leading to gingivitis and periodontitis.
Signs of gingivitis can vary depending on the severity of the disease. The gingival tissue will look reddened and swollen. The inflamed tissue may be just along the margin next to a single tooth or it can be along multiple teeth in the mouth. More severe cases of gingivitis may have inflammation extending across the entire width of the gingiva, across multiple teeth. The gingiva will appear irritated and may even bleed when touched or when the patient eats. With a closer look, the gingiva can lose that smooth appearance and appear roughened.
Preventing and Treating Gum Disease
If any evidence of gingivitis and/or calculus is present in our patient’s mouth then it is time for a COHAT. Gingivitis is reversible and the treatment includes ultrasonic scaling and polishing of the teeth above and below the gumline. Treatment is focused below the gingival margin, removing any plaque and bacteria around the teeth and under the gumline.
A COHAT treats the present disease and becomes a starting point for the continued care of our pet’s oral cavity. Continued treatment is something we strongly encourage of everyone. It includes home care options which we are happy to discuss and have also covered in earlier blog posts. Daily tooth brushing is the gold standard we should all strive for with our pets.
Remember, after a COHAT, the process of periodontal disease starts over again, almost immediately. As soon as oral bacteria and saliva contact the teeth and gingiva, plaque starts forming. Fortunately, daily brushing will disrupt this plaque formation and stop the progression of periodontal disease in most cases. Daily dental home care combined with regular COHAT procedures will keep your pet free from this prevalent and painful disease.
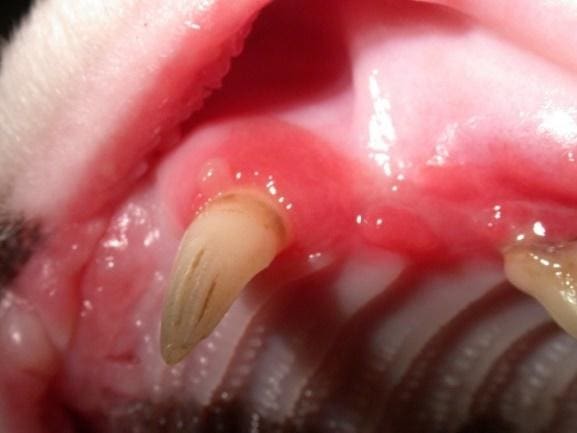
Figure 1. Healthy gingiva. No evidence of gingivitis.
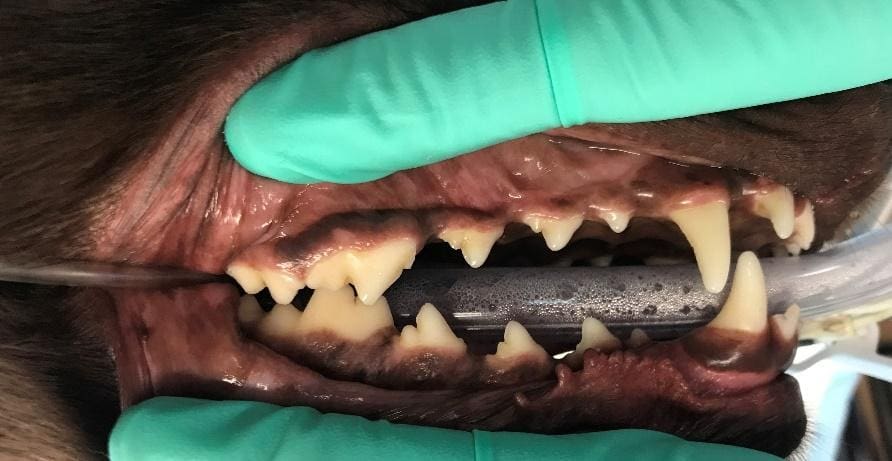
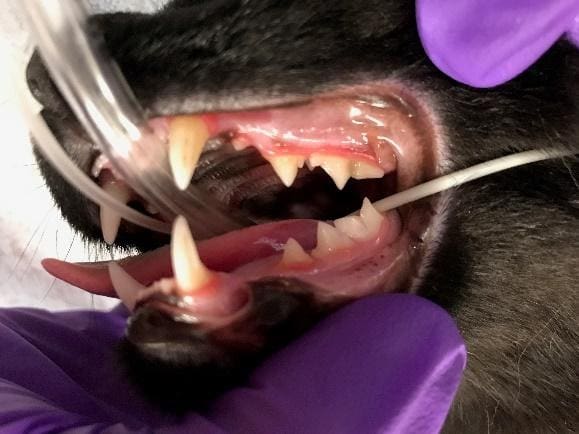
Figure 2. Gingivitis. Note the inflammation, reddening and swelling. A Comprehensive Oral Health Assessment and Treatment (COHAT) is recommended when evidence of gingivitis is present.
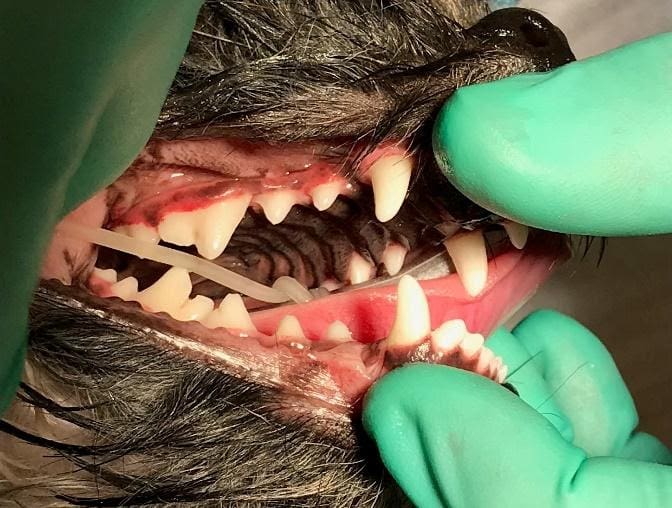
Figure 3. Examples of advanced gingivitis. Periodontal disease may or may not be present. A Comprehensive Oral Health Assessment and Treatment (COHAT) is recommended.
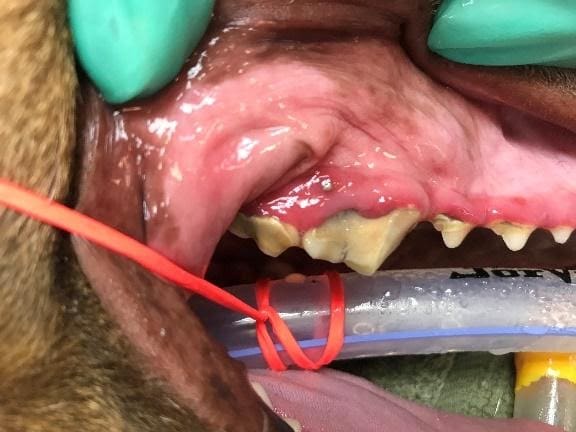
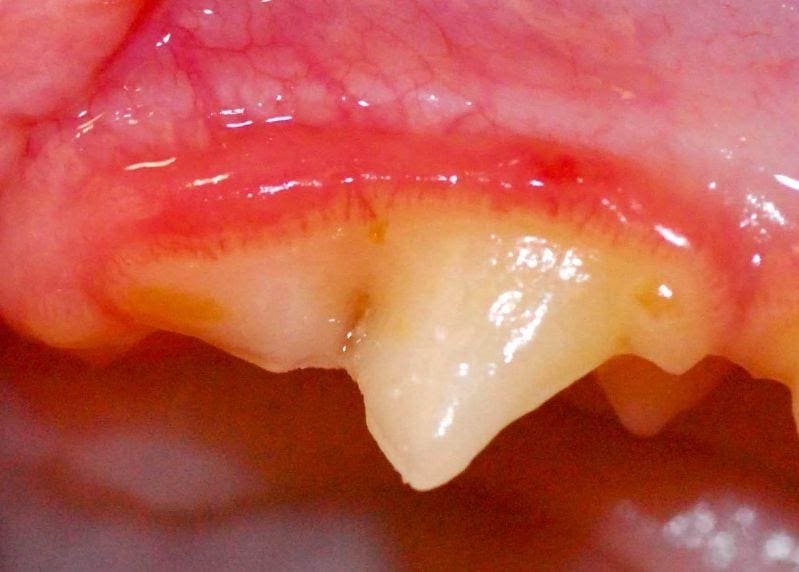
Does your dog in Castle Rock, Colorado Springs or Loveland, CO have unhealthy gums?
Contact us today at (719) 536-9949!
Image by Светлана Бердник from Pixabay (11/28/2019)


