
17 Aug Jaw Fractures in Dogs: Causes & Treatments
Jaw fractures occur in a split second and are always traumatic for both the pet and the pet owner. A broken jaw may involve both the maxilla (upper jaw) or mandible (lower jaws), however, they more frequently involve the mandible. For the sake of this discussion, I will focus on mandibular fractures.
What Causes Broken Jaws in Dogs?
At Animal Dental Care and Oral Surgery, most mandibular fractures treated have occurred because of a trauma or as a result of periodontal disease. Common traumatic events include vehicular trauma or an altercation with another dog.
Broken jaws resulting from periodontal disease are often seen near the mandibular 1st molar tooth due to severe bone loss around the tooth. The bone loss weakens the mandible, predisposing it to fracture when the patient does something as simple as jumping off a piece of furniture or biting down on a piece of hard kibble.
In the case of vehicular trauma or altercation with another dog, it is important to have your pet fully evaluated for other injuries. When the fracture occurs or is noticed it is always best to have your pet seen by your regular veterinarian or emergency clinician. Once the patient is stabilized or treated for other life-threatening injuries, the jaw fracture can be addressed.
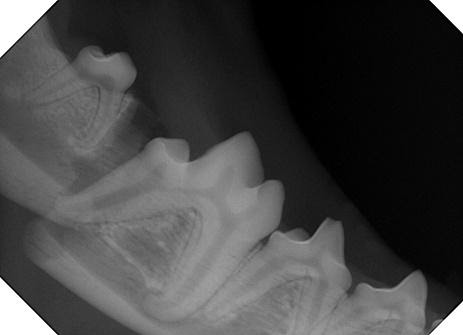
Figure 1. Radiograph of a dog’s mandible after it has been fractured during an altercation with another dog
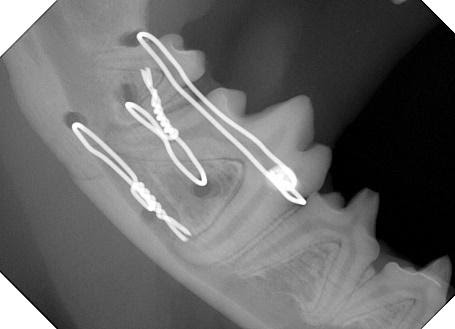
Figure 2. Radiograph of the same dog’s mandible after fixation with transosseous wires.
Treating Jaw Fractures in Dogs
Obtaining a good history of the patient and performing a thorough physical exam are always the starting point. Once the patient has been examined, the initial diagnostics (blood work, radiographs, etc..) have been completed, and the patient is stable, we can start to fully assess the jaw fracture.
Skull radiographs are often a part of the initial assessment of the fracture, and although these can provide valuable initial information, additional diagnostic imaging will be needed. Once the patient is stable an anesthetized or sedated an oral exam can be performed by your regular veterinarian, emergency clinician or veterinary dentist to fully assess the oral cavity and fracture.
In addition, diagnostics including dental radiographs and/or a CT scan (cone beam CT scan or helical CT scan) are performed to assess the fracture site and teeth involved while under anesthesia. Animal Dental Care and Oral Surgery in Colorado Springs is proud to be the only veterinary practice in Colorado with cone beam computed tomography capability.
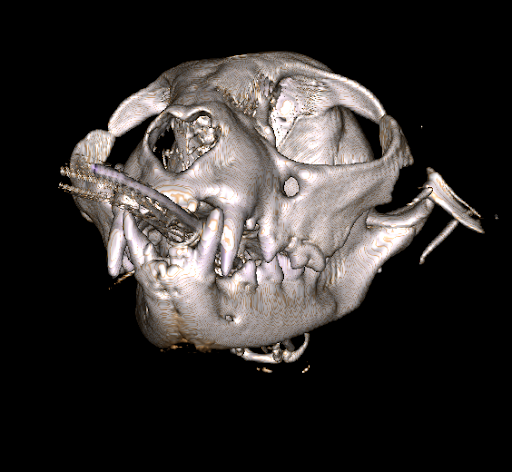
Figure 3. Three-dimensional reconstruction from cone computed tomography scan of a cat with a fracture of its zygoma bone. The fracture was the result of being attacked by a dog. The CBCT scan was completed at Animal Dental Care and Oral Surgery in Colorado Springs.
The goal of fracture repair is to create a functional reduction and alignment of the fracture using a rigid fixation to obtain a bony union across the fracture. We want to restore a normal occlusion for the patient and maintain a healthy dentition, preventing damage to the remaining teeth during the fracture repair when possible. Information including the fracture location, number of fractures, direction of the fracture line, teeth involved, oral lacerations, bone exposure and condition of the surrounding oral tissues are all important for planning the fracture repair. Our primary goal is always focused on the patient’s quality of life.
Numerous techniques may be used to stabilize a jaw fracture. The technique is usually determined once the fracture has been characterized. Oversized muzzles are used to either hold the patient in occlusion until the fracture is further stabilized or is used as the primary form of fracture stabilization. Interdental splints using wire and composite material around the crowns of the teeth, encircling cerclage wires around the mandibles, and intraosseous wires across a fracture are all techniques used to stabilize a jaw fracture.
Oral lacerations are commonly associated with jaw fractures. Any lacerations or wounds will also need to be cleaned and sutured as part of the treatment.
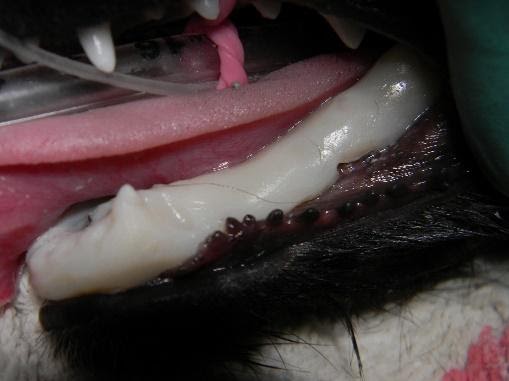
Figure 4. Acrylic composite material that has been used to stabilize a jaw fracture. The acrylic is left in place for 4-8 weeks
Taking Care of Your Dog after Jaw Surgery
After repairing the fracture, detailed instructions will be discussed regarding home care for the patient. Patients need to be confined and kept on leash to minimize running, playing or jumping around while they heal. Regardless of the type of repair technique used, we often instruct pet owners to feed a soft diet or food made into a gruel-like consistency to minimize forces and motion around the fracture.
Some patients will need a feeding tube initially while they adapt to their new situation. Feeding tubes can sound daunting to pet owners, however, most patients adjust quickly and tolerate the feeding tube very well. Detailed instructions for the feeding tube including how to use it, care for it, and specific feeding instructions are always fully discussed and written down for reference.
Lastly, depending on the method used to repair the fracture, one last anesthetized procedure needs to be scheduled to remove the wire or splint in the mouth.
Are There Complications to Treating a Broken Jaw?
Complications can be encountered when treating jaw fractures. Common complications include, infection, tearing of sutures, malalignment of the healing fracture, or instability of the fracture site leading to a malunion or nonunion of the fracture. Frequent checkup exams are scheduled to observe for complications and monitor the healing process.
Veterinary Dentist in Colorado Springs
It is important to remember that there are always options when it comes to treating your pet. At Animal Dental Care and Oral Surgery, we always strive for the best quality of life for your pet and want all of our patients to have a pain free and functional occlusion (bite). If you are in need of emergency dental care for your four-legged companion or simply need an annual dental cleaning, give us a call: 719-270-3075.

